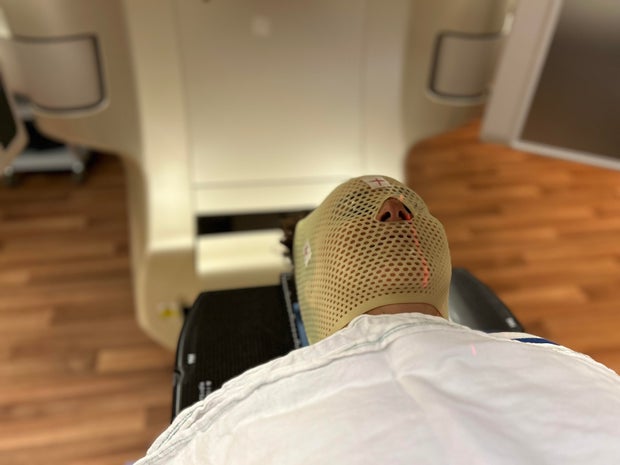
Nadya El-Afandi was nearing the end of her breast cancer treatment when she received earth-shattering news: doctors had diagnosed her with glioblastoma, a fast-growing and aggressive brain tumor.
Typical, folks diagnosed with glioblastoma die within 12 to 18 months, even with aggressive treatment options. Patients over 60 years of age usually die within six to nine months. El-Afandi was 59 when she was diagnosed in June 2023, putting her right on the edge of that worse prognosis.
“I was still on chemo, but my breast cancer doctor said, ‘You don’t have to keep taking that anymore, and you don’t have to come in for breast exams anymore,’” El-Afandi said. “He didn’t say it, but I think he said, ‘Glioblastoma is more likely to kill you than breast cancer.'”
A week after diagnosis, El-Afandi underwent surgery to remove the tumor. This is standard in the treatment of glioblastomas, but even after surgery, cancer cells usually remain due to the way the tumors grow in the brain. That’s part of the reason why the death rate for glioblastoma is so high, according to Dr. William Breen, a radiation oncologist at the Mayo Clinic and no relation to the author of this article. Even the most experienced neurosurgeon cannot remove all microscopic cells, and other treatments such as radiation and chemotherapy generally have diminishing returns in treating glioblastoma.
Two new studies are being conducted to find possible new answers. Both are led by physicians at the Mayo Clinic. One just completed its second phase and found that combining advanced imaging with a targeted form of radiation therapy extended the average lifespan of older glioblastoma patients by several months. The second is ongoing and aims to study two radiation treatment options combined with advanced imaging options. El-Afandi signed up for that second trial – and after several nerve-wracking months, her scans are clear and she is on holiday in Hawaii.
Nadya El-Afandi
“Helping other people has always been part of what I try to do, so the idea that this crappy thing that happened, something good can come out of it? I’m very happy about that,” says El-Afandi, now 61, said.
A “promising approach” to treating glioblastoma
The results of the first study were published earlier this week in the medical journal Lancet Oncology. The study, led by Dr. Sujay Vora, chairman of the department of radiation oncology at the Mayo Clinic in Arizona, investigated how proton radiation, combined with advanced imaging and a cancer drug called temozolomide, could treat glioblastomas in patients aged 65 and older.
Radiation treatment usually uses photon beams. With proton radiation, the effect is more targeted, sparing more healthy tissue, Vora explains. This, combined with more advanced imaging, allowed doctors to better target the glioblastoma. Patients in the study also had fewer radiation sessions than normal, using a higher radiation dose. Normally, radiation treatments are performed daily for six weeks, but in this study, patients had only five or 10 days of daily sessions. The goal was to see how the 39 patients participating in the study fared compared to the average survival rate at six to nine months.
What happened was “a little better than we expected,” Vora said. On average, patients who participated in the study survived for 13 months. A subpopulation of patients who were more sensitive to the effects of radiation and chemotherapy lived for 22 months. Patients also reported a higher quality of life during this period.
“Overall, it’s a promising approach,” said Dr. Akila Viswanathan, chairman of the department of radiation oncology at Johns Hopkins, who was not involved in the clinical trial. “It is much easier for patients to have just five treatments than to come in every day for six weeks. From the patient’s perspective, it is a very positive approach to quality of life. I think these are promising results. ”
Laura Segall/Bloomberg via Getty Images
Future studies and development
Although Vora’s research was promising, the proposed methodology is far from the standard of care for treating older glioblastoma patients, said Dr. Helen Shih, medical director of the proton therapy program at Mass General Brigham. Larger studies need to be done, and researchers will need to determine what change in the standard of care made the difference for patients.
Proton beam therapy and some of its imaging options are also inaccessible to large portions of the population: Shih said there are only 48 centers in the United States that perform proton radiation treatments. Meanwhile, there are thousands of centers that can perform the standard photon beam treatment.
The study found that about 10% of patients experienced a symptom called radiation necrosis, when the treatment creates dead tissue. Most of those patients were treated with steroids, Vora said, and one patient had to have necrotic tissue surgically removed. But none of the patients were hospitalized or died from the condition, he said. Radiation necrosis also occurs with normal radiation treatments, but the higher radiation doses and shorter timeline for treatment may explain why this rate was higher, Viswanathan said.
Ongoing research to “build on the work”
A second trial, also through the Mayo Clinic, aims to “build on the work” of Vora’s trial, Breen said. The study aims to enroll approximately 170 patients in Minnesota, Florida and Arizona. It again uses advanced imaging techniques to target the brain more precisely. Patients will receive the shorter proton radiation cycle or a longer course of more traditional photon radiation, to determine whether the shorter course of radiation is as safe and as effective as the traditional six weeks of treatment, Breen said.
Whatever radiation is used, the imaging technology allows doctors to “treat a tighter, smaller part of the brain,” Breen said. The trial is ongoing and Breen said results will likely be available in about three years. After her surgery in June 2023, El-Afandi was given the opportunity to register for the trial. She underwent six weeks of radiation with the standard photon treatment. She said she felt tired during that time, but was used to some of the side effects of her experience with breast cancer.
Nadya El-Afandi
“It never stopped me,” El-Afandi said. “I just continued gardening and sitting on my porch and visitors would come and hang out with me.”
During her first follow-up appointments, doctors observed inflammation in areas of her brain. After her third scan in August 2024, the scan looked “great and clear,” El-Afandi said, with no signs of glioblastoma or inflammation, more than a year after she was first diagnosed with the condition. Breen, who was involved in El-Afandi’s care, added that her “scans look great” and described her current health and quality of life as an “ideal scenario” for someone being treated for glioblastoma.
Every three months, El-Afandi has a new series of imaging done to monitor the growth of a glioblastoma, but in the meantime she spends time with her husband and four children and “goes on adventures as a family,” she said.
“I’m 17 months removed from diagnosis and feeling great,” she told CBS News, from the Hawaiian catamaran where she was doing her snorkeling expedition. “Every day is a gift.”