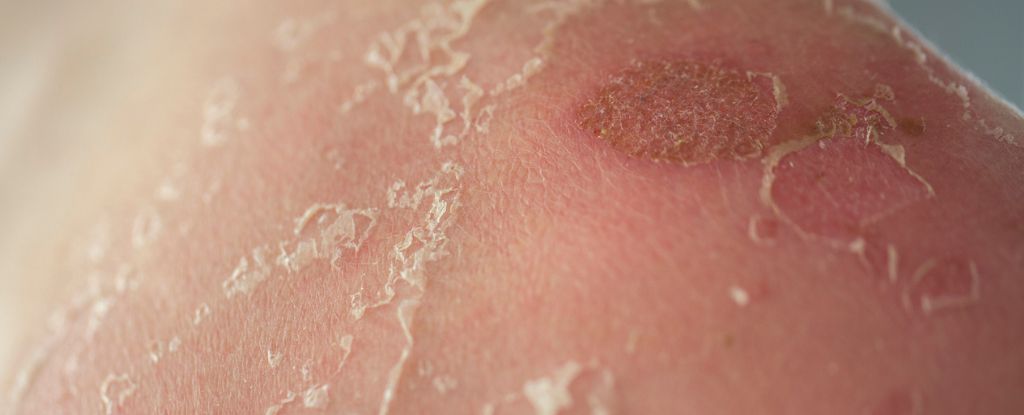
A rare and potentially fatal skin infection with nightmarish consequences could soon be cured.
The infection starts as a seemingly harmless rash, and before a person knows it, more than 30 percent of the skin on their body begins to blister and peel, usually starting on the face and chest, before progressing to the mouth , eyes, and genitals.
Infections, organ failure and pneumonia can quickly follow. The condition is fatal in a third of all cases. For those who survive, recovery can take months and usually requires similar treatment to burn victims.
The debilitating infection is an immune reaction to medication called toxic epidermal necrolysis (TEN), and while it is fortunately very rare, affecting a million or two people worldwide every year, its onset is highly unpredictable.
TEN is linked to more than 200 medications and can affect all age groups and ethnicities, although it is more common in women than men and 100 times more common in people with human immunodeficiency virus (HIV).
An international team of researchers, led by biochemists from the Max Planck Institute in Germany, now claims to have cured seven patients with TEN or a slightly less severe version of the infection known as Stevens-Johnson syndrome (SJS). None of the patients reported side effects.
“I am beyond proud of this incredible research collaboration that has already helped save the lives of multiple patients,” said biomedical researcher Holly Anderton of the Walter and Eliza Hall Institute of Medical Research in Australia.
“All seven people treated with this therapy in our study experienced rapid improvement and a full recovery, with stunning results that likely unlocked a cure for the condition.”
One of those patients was a 59-year-old man who developed TEN over 35 percent of his body after starting treatment for lung cancer. The patient had lost so much skin that his predicted mortality risk was almost 60 percent.
However, when he took a new immune blocker, his infection stopped progressing. After 16 days he was almost completely healed.
This class of drugs, called JAK inhibitors (JAKi), appears to work by suppressing an overactive immune pathway.
Scientists discovered the importance of this signaling pathway using skin samples from patients with TEN to see which individual cells caused the deadly disease. In total, they identified six proteins involved in the JAK/STAT pathway that are upregulated in people with the skin infection.
The JAK/STAT pathway is the leading cause of skin inflammation, damaged skin cells and epidermis detachment.
Using rodent models of TEN, researchers found that one to three days after taking an oral JAK inhibitor, skin infections were noticeably improved.
“Based on our compelling preclinical data and the urgent clinical need for this devastating disease, we treated seven patients with TEN or SJS-TEN overlapping with JAKi off-label,” writes the team of researchers, led by biochemist Thierry Nordmann of the Max Planck Institute.
All seven patients responded well to treatment and were discharged in good health, paving the way for a future clinical trial.
“It can take a patient weeks to recover from the damage, even after stopping taking the medication that caused the side effect,” says Anderton.
“Being able to quickly halt the progression of this disease, as we saw in our study, will make a huge difference in the standard of care for patients diagnosed with this life-threatening condition.”
The research was published in Nature.